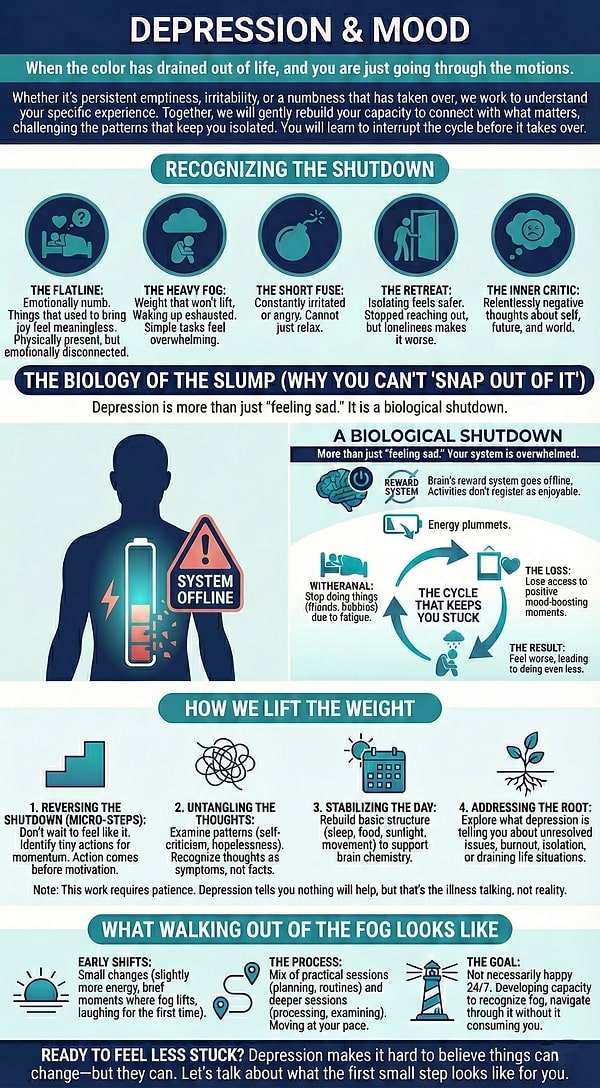
Depression & Mood

Recognizing the Shutdown
- The Flatline: You feel emotionally numb. Things that used to bring you joy – hobbies, music, friends – feel meaningless now. You are physically present, but emotionally disconnected.
- The Heavy Fog: There is a weight that won’t lift. You wake up feeling exhausted before the day even starts, and simple tasks (like showering or texting back) feel overwhelming.
- The Short Fuse: Instead of sadness, you feel constantly irritated or angry. People tell you to “just relax,” but you can’t.
- The Retreat: Isolating feels safer than pretending you’re okay. You’ve stopped reaching out to people, but the loneliness is making everything worse.
- The Inner Critic: Your thoughts have become relentlessly negative – about yourself (“I’m lazy”), your future (“It won’t get better”), and the world.
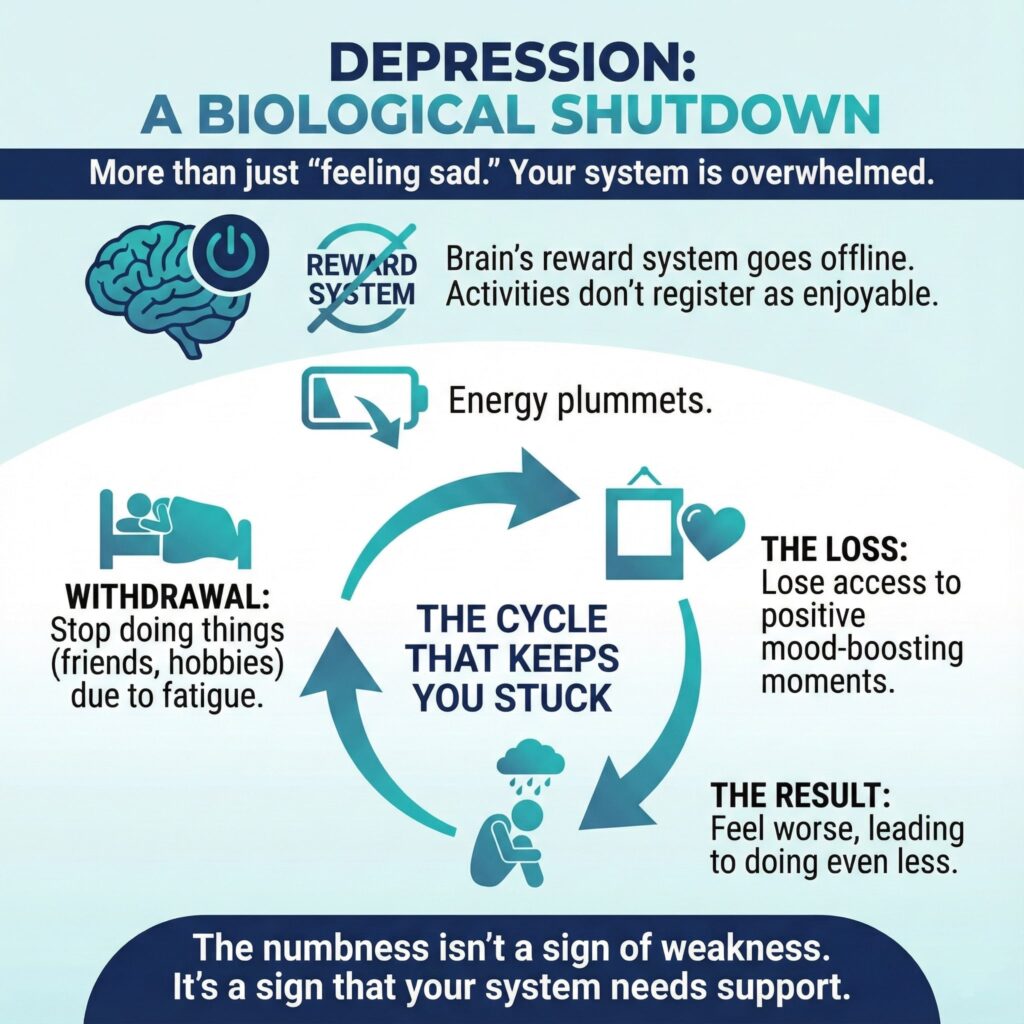
The Biology of the Slump (Why You Can't "Snap Out of It")
- Withdrawal: You feel tired, so you stop doing things (like seeing friends, exercising, and hobbies).
- The Loss: You lose access to the positive moments that usually boost your mood.
- The Result: You feel worse, which makes you want to do even less.

How We Lift the Weight
- Reversing the Shutdown (Micro-Steps) We don’t wait until you “feel like” doing things to start moving because the motivation won’t come while you are sitting still. We identify micro-steps, tiny, manageable actions that create a spark of momentum. Action comes before motivation.
- Untangling the Thoughts We examine the thought patterns that fuel the fog, self-criticism, hopelessness, and all-or-nothing thinking. You’ll learn to recognize these thoughts as symptoms of depression, not facts about your character.
- Stabilizing the Day Depression erodes your routine. We work on gently rebuilding the basic structure – sleep, food, sunlight, movement – that supports your brain chemistry, even when you don’t feel like it.
- Addressing the Root Sometimes depression is a response to something real – unresolved grief, chronic stress, burnout, isolation, or being stuck in a life situation that’s draining you. We explore what your depression might be trying to tell you about what needs to change in your life.

Ready to Feel Less Stuck?
Depression makes it hard to believe things can change, but they can. Let's talk about what the first small step looks like for you.
$150 per 50-minute session - Insurance billing available
What Walking Out of the Fog Looks Like
Recovery from depression is gradual. It is rarely a straight line.
Early Shifts
You might first notice small changes: slightly more energy on some days, brief moments where the fog lifts, or realizing you laughed at a joke for the first time in months.
The Process
Some sessions will be practical: planning your week, building routines. Others will be deeper: processing grief, examining what is keeping you stuck. We move at your pace.
The Goal
You won't necessarily be happy 24/7. But you will develop the capacity to recognize when the fog is rolling in, and you will have the tools to navigate through it so it doesn't consume you.

Page Summary
Frequently Asked Questions About Depression Counselling
How do I know if I should see a therapist about my depression symptoms?
You don’t need to wait until you’re in crisis to start therapy. If depression is affecting your daily life, lasting more than two weeks, or causing you significant distress, counselling can help. Early intervention typically leads to better outcomes.
Common signs you should seek help
- Persistent low mood or sadness lasting most days
- Loss of interest in activities you once enjoyed
- Changes in sleep (insomnia or oversleeping)
- Changes in appetite or weight
- Difficulty concentrating or making decisions
- Feelings of worthlessness or excessive guilt
- Fatigue or loss of energy
- Thoughts of death or suicide
Crisis Resources
If you’re experiencing thoughts of suicide or self-harm: Call 1-800-SUICIDE (1-800-784-2433) immediately.
Seek emergency support for: inability to care for yourself, substance use to cope, or psychotic symptoms (hearing voices, severe paranoia).
Related questions What are the most common signs and symptoms of depression? • Can therapy help without medication? • What happens in a first session?
Book your first session to discuss whether counselling is right for your depression symptoms.
References
American Psychiatric Association. (2022). Diagnostic and statistical manual of mental disorders (5th ed., text rev.). https://doi.org/10.1176/appi.books.9780890425787
Cuijpers, P., Miguel, C., Harrer, M., Plessen, C. Y., Ciharova, M., Ebert, D., & Karyotaki, E. (2023). Cognitive behavior therapy vs. control conditions, other psychotherapies, pharmacotherapies and combined treatment for depression: A comprehensive meta-analysis including 409 trials with 52,702 patients. World Psychiatry, 22(1), 105-115. https://doi.org/10.1002/wps.21069
What does a typical first counselling session for depression look like?
Your first depression counselling session is a conversation, not an interrogation. We’ll discuss what brings you to therapy, your depression symptoms and their impact on your life, previous treatment experiences (if any), and your hopes for counselling. I’ll explain how therapy works, answer your questions about confidentiality and the process, and begin developing a treatment approach together. You control what you share and the pace we move at.
Session Timeline (50 minutes total)
Minutes 0-15: Building Rapport & Safety
We start wherever feels comfortable for you. No pressure to share everything immediately.
Minutes 15-40: Understanding Your Depression
We explore your symptoms, their impact on daily life, and what brought you to therapy now.
Minutes 40-50: Next Steps & Questions
We discuss how therapy works, answer your questions about confidentiality, and outline a treatment approach.
Case Study (Composite scenario for educational purposes):
James, 41, arrived visibly anxious. “I don’t know what you need to know,” he said. I explained we’d start wherever felt comfortable for him and that he could skip anything that felt too personal. We spent twenty minutes building rapport before he shared that depression had affected his marriage and work for six months. By the end, James said, “I was dreading this, but it felt surprisingly normal.”
You don’t need to
- Have your whole life story prepared
- Know exactly why you’re depressed
- Cry or show intense emotion
- Make immediate long-term commitments
- Share anything you’re uncomfortable discussing
After the first session, we’ll both reflect on whether we’re a good fit. Most clients feel ready to continue, but if you have concerns, we’ll discuss them openly. You’re never locked into working with any therapist.
Related questions How does depression therapy actually work? • How long until I notice changes? • Do I need a doctor’s referral?
Policy details Informed Consent • Privacy & Confidentiality
Book your first session and see what depression counselling actually looks like.
References
Herman, J. L. (2015). Trauma and recovery: The aftermath of violence; from domestic abuse to political terror. Basic Books.
Norcross, J. C., & Lambert, M. J. (2018). Psychotherapy relationships that work III. Psychotherapy, 55(4), 303-315. https://doi.org/10.1037/pst0000193
Do I need a doctor's referral to see a counsellor for depression in BC?
No, you do not need a doctor’s referral to start depression counselling in British Columbia. You can book directly with a registered counsellor like those at Introspectus Counselling in Greater Victoria. Some insurance plans may require a doctor’s note for extended benefits coverage, but this is plan-specific, not a legal requirement.
BC operates on a self-referral model for mental health counselling, meaning you can access therapy directly without seeing a family doctor first. This reduces barriers and allows you to start treatment immediately.
When You Might Want to See Your Doctor First
- To rule out medical causes of depression (thyroid problems, vitamin D deficiency, medication side effects)
- To discuss whether medication might be appropriate alongside therapy
- To get a formal diagnosis if your insurance requires one
- To access publicly-funded services through health authority referrals
If your insurance requires a doctor’s note, this is typically simple. Your family doctor can provide a letter stating you would benefit from counselling for depression; you don’t need a formal psychiatric evaluation.
Private vs. Public Mental Health Services in BC
Private Counselling (Introspectus)
- Referral Required: No
- Wait Time: 1-2 weeks
- Cost: $150/session (often insurance-covered)
- Therapist Choice: You choose based on specialization
- Session Availability: Flexible scheduling
Public Services (Island Health)
- Referral Required: Sometimes (program-dependent)
- Wait Time: Weeks to months
- Cost: Free
- Therapist Choice: Assigned (may be students or rotating therapists)
- Session Availability: Limited availability
The Benefit of Direct Access
- Faster care when you need it
- Ability to choose a therapist whose specialization matches your needs
- No waiting for medical appointments
- Control over whether your depression is documented in medical records
Collaboration with Your Doctor
Even though a referral isn’t required, many clients benefit from coordinated care between their counsellor and family doctor, especially if medication is being considered, medical conditions contribute to depression, or you’re experiencing severe symptoms. With your written consent, I can communicate with your doctor to ensure comprehensive care.
Related questions Session costs and payment • Is counselling covered by insurance? • What happens in a first session?
Policy Informed Consent • Privacy (Sharing with Healthcare Providers)
Ready to start without waiting? Book your first session today.
References
BC Association of Clinical Counsellors. (2023). Access to counselling services in British Columbia. https://bcacc.ca/
Can talk therapy alone help with depression, or do I always need medication too?
Yes, talk therapy alone is highly effective for mild to moderate depression. Research shows that Cognitive Behavioral Therapy and Acceptance and Commitment Therapy produce outcomes comparable to antidepressant medication, with the advantage of developing lasting skills that prevent relapse. Many people successfully manage depression with therapy alone.
For moderate to severe depression, combining therapy and medication often produces the best results, though this isn’t always necessary. The right approach depends on your depression severity, previous treatment responses, personal preferences, and whether you have access to quality therapy.
At Introspectus Counselling in Greater Victoria, we use ACT to help clients develop psychological flexibility and reduce depressive symptoms; many clients achieve meaningful recovery without medication.
Case Study (Composite scenario for educational purposes):
Maria, 28, had negative experiences with antidepressants and wanted to try therapy first. “I’m worried you’ll tell me I need medication,” she said. We discussed how ACT helps people change their relationship with depressive thoughts rather than requiring chemical intervention. After 16 sessions, her PHQ-9 depression score dropped from 18 (moderately severe) to 7 (mild). She never needed medication.
When therapy alone often works well
- ✓ Mild to moderate depression (not severe)
- ✓ Can function in daily life with support
- ✓ Prefer non-medication approaches
- ✓ Previous unsuccessful medication trials or significant side effects
- ✓ Committed to active therapy participation
When combined therapy and medication may help
- Depression is severe or treatment-resistant
- Significant functional impairment or suicide risk
- Co-occurring conditions (anxiety, bipolar disorder)
- Preference for combined approach
Important I cannot prescribe or adjust medication, but I can collaborate with your family doctor or psychiatrist when medication is part of your treatment plan. You always maintain the right to make informed decisions about your care and the ability to share your information with other professionals.
Related questions How does depression therapy work? • Will I feel like myself again? • How long until I notice changes?
Learn more Acceptance and Commitment Therapy • Mindfulness Therapy • Depression Counselling
Book your first session to discuss whether therapy alone or combined treatment is right for you.
References
American Psychological Association. (2019). Clinical practice guideline for the treatment of depression across three age cohorts. https://www.apa.org/depression-guideline
Cuijpers, P., Karyotaki, E., de Wit, L., & Ebert, D. D. (2021). The effects of fifteen evidence-supported therapies for adult depression: A meta-analytic review. Psychotherapy Research, 31(8), 940-954. https://doi.org/10.1080/10503307.2020.1860143
What actually happens in depression therapy sessions?
Depression therapy at Introspectus Counselling uses Acceptance and Commitment Therapy (ACT), an approach that helps you build a meaningful life even while managing depression symptoms. Rather than focusing solely on eliminating negative thoughts, ACT teaches you to notice depressive thoughts without being controlled by them, identify what matters most to you (your values), and take action aligned with those values even when depression is present.
Research shows ACT is as effective as traditional CBT with longer-lasting results.
What ACT looks like in practice
Instead of arguing with the thought “I’m worthless,” you practice noticing: “I’m having the thought that I’m worthless.” This creates distance (called “defusion”) between you and your thoughts, allowing you to choose valued actions regardless of what your mind says.
Example of values-based action
If being a present parent is a core value, you attend your child’s soccer game even when depression says you’re “too tired.” The behavioral activation reduces depression more effectively than debating the thought.
Case Study (Composite scenario for educational purposes):
David, 52, struggled with persistent thoughts of worthlessness. Rather than debating whether the thought was true, we practiced defusion: noticing the thought without getting tangled in it. David identified being a present father as a core value. Despite depression telling him he was “too tired,” he started attending his daughter’s soccer games. The behavioral activation and values-based action reduced his depression more effectively than years of arguing with his thoughts.
What to expect in therapy
Early Sessions (1-6) Understanding your depression and identifying your core values
Middle Sessions (7-14) Building skills in mindfulness, defusion (separating yourself from thoughts), and values-based action
Later Sessions (15-20) Consolidating new patterns and preparing for future challenges
Therapy typically lasts 12-20 sessions for depression, though timelines vary based on individual needs.
Between sessions, you’ll practice brief skills: 5-10 minutes of mindfulness, noticing thought patterns, and experimenting with valued activities. We track progress using standardized measures like the PHQ-9 depression scale alongside your subjective experience of mood and functioning.
Related questions What happens in a first session? • How long until I notice changes? • Can therapy work without medication?
Learn more Acceptance and Commitment Therapy • Mindfulness Therapy • Depression Counselling
Book your first session to experience how ACT-based depression counselling works.
References
A-Tjak, J. G., Davis, M. L., Morina, N., Powers, M. B., Smits, J. A., & Emmelkamp, P. M. (2015). A meta-analysis of the efficacy of acceptance and commitment therapy for clinically relevant mental and physical health problems. Psychotherapy and Psychosomatics, 84(1), 30-36. https://doi.org/10.1159/000365764
Hayes, S. C., Strosahl, K. D., & Wilson, K. G. (2012). Acceptance and commitment therapy: The process and practice of mindful change (2nd ed.). Guilford Press.
How long does it typically take to see changes with depression therapy?
Most clients notice initial improvements in depression symptoms within 4-8 sessions, with significant change typically occurring over 12-20 sessions. However, timelines vary based on depression severity, how long you’ve been depressed, co-occurring issues, and individual differences in treatment response.
Recovery is rarely linear; expect ups and downs as you develop new skills. Some weeks you’ll feel better, others worse. This doesn’t mean therapy isn’t working.
Recovery Timeline
Weeks 1-4: Early Changes
- Increased hope from having support
- Better understanding of your depression patterns
- Beginning skill development (mindfulness, noticing thoughts)
- Some notice slight mood improvements; others don’t yet
Weeks 5-12: Building Momentum
- More consistent mood improvements
- Increased behavioral activation (doing valued activities despite low motivation)
- Reduced impact of depressive thoughts
- Better sleep, appetite, or energy in some areas
Weeks 13-20: Consolidation
- Sustainable symptom reduction
- Stronger skills in managing depression triggers
- Clearer sense of values and purpose
- Increased confidence in handling difficult emotions
Case Study (Composite scenario for educational purposes):
Karen, 45, asked in session 6: “I don’t feel better yet. Is this working?” We reviewed her PHQ-9 scores: she’d gone from 19 (moderately severe) to 14 (moderate) without realizing it. She was sleeping better and crying less frequently, though she still felt “depressed.” By session 14, Karen reported: “I’m not completely better, but I’m functioning. I didn’t think that was possible.”
Signs Therapy Is Working (Even If You Don’t “Feel Better” Yet)
- ✓ Increased understanding of depression patterns
- ✓ Using skills more consistently (noticing thoughts, practicing mindfulness)
- ✓ Small behavioral changes (taking walks, calling friends, cooking meals)
- ✓ Reduced intensity of depressive episodes
- ✓ Quicker recovery from low mood
- ✓ More self-compassion for struggles
Factors That Influence Timeline
Faster Progress Often Occurs With
- Mild to moderate depression (not severe)
- Recent onset (months not years)
- Strong therapeutic relationship
- Active engagement in between-session practices
- Stable life circumstances
Longer Treatment May Be Needed For
- Severe or long-standing depression
- History of trauma or adverse childhood experiences
- Co-occurring mental health conditions
- Ongoing life stressors (relationship conflict, job loss)
- Previous unsuccessful treatment attempts
If you’re not noticing any changes after 8-10 sessions, we’ll reassess goals and treatment approach, consider whether additional support is needed (medication evaluation, more intensive therapy), discuss whether a different therapist might be more effective, and rule out medical causes of depression.
Related questions How does depression therapy work? • Can therapy work without medication? • Will I feel like myself again?
Learn more Acceptance and Commitment Therapy • Depression Counselling
Book your first session to begin working toward meaningful change.
References
American Psychological Association. (2019). Clinical practice guideline for the treatment of depression across three age cohorts. https://www.apa.org/depression-guideline
Twohig, M. P., & Levin, M. E. (2017). Acceptance and commitment therapy as a treatment for anxiety and depression: A review. Psychiatric Clinics of North America, 40(4), 751-770. https://doi.org/10.1016/j.psc.2017.08.009
How much does depression therapy cost, and is there a sliding scale?
Session Cost $150 for 50 minutes (typical for registered counsellors in Greater Victoria)
Insurance Coverage Most extended health insurance plans covering Canadian Certified Counsellors reimburse 50-100% of session costs, significantly reducing your out-of-pocket expense.
Check Your Coverage (5 Questions to Ask Your Insurer)
- “Does my plan cover a Canadian Certified Counsellor (CCC)?”
- “What is my annual maximum for counselling?”
- “What percentage is reimbursed per session?”
- “Is there a per-session dollar limit?”
- “Do I need a referral or pre-authorization?”
BC Insurers That Typically Cover CCCs
Major Providers Pacific Blue Cross, Sun Life Financial, Manulife, Great-West Life, Canada Life, Green Shield Canada
Additional Providers Chambers of Commerce Group Insurance, ASEBP, Industrial Alliance, SSQ Insurance, Desjardins Insurance, and whatever other plan covers Canadian Certified Counsellors
How Payment Works
- Step 1 You pay the full $150 session fee at time of service
- Step 2 I provide a detailed receipt with my CCC registration number
- Step 3 You submit the receipt to your insurance company
- Step 4 Your insurer reimburses you (typically within 1-2 weeks)
Financial Options If You Don’t Have Insurance
- Use a Health Spending Account (HSA) if available through your employer
- Claim counselling as a medical expense on your tax return (CRA allows this)
- Space sessions biweekly instead of weekly to reduce monthly costs
- Focus on shorter-term therapy (12-16 sessions) for specific goals
Important BC Distinction
MSP (Medical Services Plan) does NOT cover counselling. MSP only covers psychiatrists.
Extended Health Benefits (private insurance through employers) typically cover registered counsellors including CCCs, RCCs, Registered Psychologists, and Clinical Social Workers.
Related questions Do I need a doctor’s referral? • What happens in a first session? • Can insurers access my therapy details?
Policy Fees & Billing • Cancellation Policy • Privacy (Insurance Billing)
Questions about costs or insurance? Book your first session and bring your benefits booklet; we can review it together.
References
Canadian Counselling and Psychotherapy Association. (2023). Find a Canadian Certified Counsellor: Insurance coverage. https://www.ccpa-accp.ca/find-a-canadian-certified-counsellor/
Canadian Life and Health Insurance Association. (2021). Canadian life and health insurance facts: 2021 edition. https://www.clhia.ca/web/clhia_lp4w_lnd_webstation.nsf/page/ECB5C0C38583D54685257F1B00542C0A
Does insurance cover depression counselling?
Session Cost $150 for 50 minutes (typical for registered counsellors in Greater Victoria)
Insurance Coverage Most extended health insurance plans covering Canadian Certified Counsellors reimburse 50-100% of session costs, significantly reducing your out-of-pocket expense.
Check Your Coverage (5 Questions to Ask Your Insurer)
- “Does my plan cover a Canadian Certified Counsellor (CCC)?”
- “What is my annual maximum for counselling?”
- “What percentage is reimbursed per session?”
- “Is there a per-session dollar limit?”
- “Do I need a referral or pre-authorization?”
BC Insurers That Typically Cover CCCs
Major Providers Pacific Blue Cross, Sun Life Financial, Manulife, Great-West Life, Canada Life, Green Shield Canada
Additional Providers Chambers of Commerce Group Insurance, ASEBP, Industrial Alliance, SSQ Insurance, Desjardins Insurance, and whatever other plan covers Canadian Certified Counsellors
How Payment Works
- Step 1 You pay the full $150 session fee at time of service
- Step 2 I provide a detailed receipt with my CCC registration number
- Step 3 You submit the receipt to your insurance company
- Step 4 Your insurer reimburses you (typically within 1-2 weeks)
Financial Options If You Don’t Have Insurance
- Use a Health Spending Account (HSA) if available through your employer
- Claim counselling as a medical expense on your tax return (CRA allows this)
- Space sessions biweekly instead of weekly to reduce monthly costs
- Focus on shorter-term therapy (12-16 sessions) for specific goals
Important BC Distinction
MSP (Medical Services Plan) does NOT cover counselling. MSP only covers psychiatrists.
Extended Health Benefits (private insurance through employers) typically cover registered counsellors including CCCs, RCCs, Registered Psychologists, and Clinical Social Workers.
Related questions Do I need a doctor’s referral? • What happens in a first session? • Can insurers access my therapy details?
Policy Fees & Billing • Cancellation Policy • Privacy (Insurance Billing)
Questions about costs or insurance? Book your first session and bring your benefits booklet; we can review it together.
References
Canadian Counselling and Psychotherapy Association. (2023). Find a Canadian Certified Counsellor: Insurance coverage. https://www.ccpa-accp.ca/find-a-canadian-certified-counsellor/
Canadian Life and Health Insurance Association. (2021). Canadian life and health insurance facts: 2021 edition. https://www.clhia.ca/web/clhia_lp4w_lnd_webstation.nsf/page/ECB5C0C38583D54685257F1B00542C0A
Will I ever feel like myself again?
Yes. Long-term depression is treatable, and most people experience significant improvement with appropriate therapy, even after years of suffering. Recovery doesn’t always mean returning to “who you were before”; many clients discover a deeper, more resilient version of themselves through the therapeutic process. You can reclaim joy, purpose, and connection, even if depression has been present for months or years.
Acceptance and Commitment Therapy (ACT), used at Introspectus Counselling in Greater Victoria, helps you build a meaningful life even while managing depression symptoms. Research shows 60-70% of individuals with chronic depression (lasting 2+ years) respond well to evidence-based psychotherapy.
What Recovery Actually Means
Rather than eliminating depression entirely, therapy helps you:
- ✓ Experience positive emotions more frequently and intensely
- ✓ Take valued actions even when motivation is low
- ✓ Notice thoughts and feelings without being controlled by them
- ✓ Build a life worth living alongside managing ongoing symptoms
- ✓ Develop self-compassion for continuing struggles
Case Study (Composite scenario for educational purposes):
Linda, 58, began therapy after 10 years of persistent depression. “I don’t even remember what ‘normal’ feels like,” she said. Through ACT-based treatment, Linda learned to engage in valued activities (gardening, time with grandchildren) despite low mood. By session 24, she reported: “I still have hard days, but I’m living my life again. I didn’t think that was possible. I’m not the same person I was before depression, but I like who I’m becoming.”
What to Expect in Recovery
Short-Term (Weeks 1-12)
- Slightly better sleep or appetite
- Brief moments of pleasure or interest
- Reduced emotional numbness
- Increased understanding of depression patterns
- Hope that change is possible
Medium-Term (Months 3-6)
- More frequent positive emotions
- Increased behavioral activation (engaging in valued activities)
- Better relationships with self and others
- Reduced impact of depressive thoughts
- Sustainable daily functioning
Long-Term (Months 6-12+)
- Consistent mood stability with manageable fluctuations
- Strong skills in managing setbacks
- Clear sense of values and purpose
- Meaningful relationships and activities
- Acceptance of ongoing vulnerability to depression
- Confidence in managing future challenges
The Reality For some people, depression becomes a chronic condition requiring ongoing management (like diabetes or high blood pressure). This doesn’t mean you can’t live a fulfilling life; it means you develop skills to manage symptoms rather than waiting to be “cured” before living.
What Supports Faster Recovery
- Engaging actively in therapy and practicing skills between sessions
- Being patient with non-linear progress (setbacks are normal)
- Building valued activities incrementally
- Developing self-compassion for struggles
- Connecting with supportive relationships
- Addressing physical health (sleep, exercise, nutrition)
Related questions How long until I notice changes? • Can therapy work without medication? • How does depression therapy work?
Learn more Acceptance and Commitment Therapy • Depression Counselling • Mindfulness Therapy
You don’t have to stay stuck. Book your first session and begin reclaiming your life.
References
American Psychological Association. (2019). Clinical practice guideline for the treatment of depression across three age cohorts. https://www.apa.org/depression-guideline
Klein, D. N. (2010). Chronic depression: Diagnosis and classification. Current Directions in Psychological Science, 19(2), 96-100. https://doi.org/10.1177/0963721410366007
Zettle, R. D., Rains, J. C., & Hayes, S. C. (2011). Processes of change in acceptance and commitment therapy and cognitive therapy for depression: A mediation reanalysis of Zettle and Rains. Behavior Modification, 35(3), 265-283. https://doi.org/10.1177/0145445511398344
What are the most common signs and symptoms of depression?
Common depression symptoms in adults include persistent sadness or empty mood, loss of interest in activities once enjoyed, significant weight or appetite changes, sleep disturbances (insomnia or oversleeping), fatigue, feelings of worthlessness or excessive guilt, difficulty concentrating, and recurrent thoughts of death or suicide. Symptoms must persist for at least two weeks and significantly impair your functioning to meet criteria for major depression.
If you’re experiencing several of these symptoms, you’re not alone; depression is highly treatable. At Introspectus Counselling in Greater Victoria, we provide comprehensive depression assessment and treatment using Acceptance and Commitment Therapy (ACT) tailored to your unique presentation.
Depression Symptoms by Category
Emotional Symptoms
- Persistent sadness, emptiness, or hopelessness
- Irritability or frustration (especially in men)
- Feelings of worthlessness or excessive guilt
- Loss of interest in hobbies, sex, or social activities
- Emotional numbness (feeling “nothing” rather than sadness)
- Increased sensitivity to criticism or rejection
- Frequent crying or inability to cry
Cognitive Symptoms
- Difficulty concentrating or making decisions
- Memory problems
- Negative or pessimistic thinking patterns
- Rumination (repetitive negative thoughts)
- Thoughts of death, dying, or suicide
- Feeling like a burden to others
- Difficulty experiencing positive emotions or hope for the future
Physical Symptoms
- Fatigue or loss of energy
- Changes in appetite or weight (increase or decrease)
- Sleep disturbances (insomnia or hypersomnia)
- Physical aches and pains without clear medical cause
- Psychomotor changes (restlessness or slowed movements)
- Reduced libido (sex drive)
- Digestive problems
Behavioral Symptoms
- Social withdrawal or isolation
- Reduced productivity at work or school
- Neglecting personal hygiene or appearance
- Avoiding responsibilities or activities
- Substance use to cope with feelings
- Self-harm behaviors
- Difficulty initiating or completing tasks
Depression Looks Different in Different People
Men Often Experience
- Irritability or anger more than sadness
- Physical symptoms (headaches, digestive issues)
- Risk-taking behaviors
- Increased substance use
- Difficulty admitting emotional distress
Women Often Experience
- More pronounced sadness and crying
- Guilt and self-blame
- Anxiety symptoms alongside depression
- Sleep and appetite changes
- Rumination and overthinking
Older Adults Often Experience
- More physical complaints and pain
- Memory and concentration problems
- Social withdrawal
- Loss of interest in usual activities
- Less obvious mood symptoms (may not report “sadness”)
Case Study (Composite scenario for educational purposes):
Michael, 42, didn’t recognize his depression initially. He wasn’t crying or feeling “sad”; instead, he experienced intense irritability, couldn’t concentrate at work, and had unexplained back pain. His wife noticed he’d stopped playing guitar and avoided friends. When his family doctor asked about depression, Michael connected these symptoms for the first time. In therapy, he learned that depression manifests differently in different people.
When to Seek Professional Help
Seek help if:
- ☑ Symptoms persist for more than two weeks
- ☑ Symptoms interfere with work, relationships, or daily functioning
- ☑ You’re experiencing thoughts of death or suicide
- ☑ Previous coping strategies no longer work
- ☑ Physical symptoms have no medical explanation
- ☑ You’re using substances to cope with feelings
- ☑ Family or friends have expressed concern about changes in your behavior
Seek immediate help if
- You have specific plans to harm yourself
- You’re hearing voices or experiencing delusions
- You cannot care for yourself or dependents
- You’re experiencing severe impairment in functioning
Crisis Resources Call 1-800-SUICIDE (1-800-784-2433) for 24/7 crisis support or 911 for immediate danger.
Depression vs. Normal Sadness
Normal Sadness
- Tied to specific events or losses
- Improves with time and support
- Doesn’t severely impair functioning
- Allows for moments of pleasure
- Responds to positive events
Clinical Depression
- May have no clear trigger or persists long after trigger resolves
- Doesn’t improve without intervention
- Significantly impairs functioning
- Persistent inability to experience pleasure (anhedonia)
- Doesn’t respond to positive events
Related questions When should I see a therapist for depression? • Can therapy work without medication? • What happens in a first session?
Learn more Depression Counselling • Acceptance and Commitment Therapy • Mindfulness Therapy
Recognizing your symptoms is the first step toward recovery. Book your first session to discuss your depression symptoms and begin treatment.
References
American Psychiatric Association. (2022). Diagnostic and statistical manual of mental disorders (5th ed., text rev.). https://doi.org/10.1176/appi.books.9780890425787
National Institute of Mental Health. (2023). Depression: What you need to know. https://www.nimh.nih.gov/health/publications/depression
References
Nusslock, R., Alloy, L. B., Brody, G. H., & Miller, G. E. (2024). Annual Research Review: Neuroimmune network model of depression: a developmental perspective. Journal of Child Psychology and Psychiatry, 65(4), 538-567. https://doi.org/10.1111/jcpp.13961
Hoyer, J., Hoefler, M., & Wuellhorst, V. (2020). Activity and subsequent depression levels: A causal analysis of behavioural activation group treatment with weekly assessments over 8 weeks. Clinical Psychology & Psychotherapy, 27(3), 330-336. https://doi.org/10.1002/cpp.2430
Counselling for Depression That Starts Where You Are
When nothing feels meaningful anymore and life feels like you are just going through the motions, it is hard to imagine that things could be different. Maybe you are too tired to care about anything, or maybe you are functioning fine on the outside while collapsing on the inside—what some people call high functioning depression.
Sean Lewis spent a decade in pastoral ministry, including six years leading the Mustard Seed Street Church in Victoria, where hopelessness was not a clinical concept but the daily reality of people who had lost everything. He does not rush people toward positivity. He sits with the heaviness honestly, because that is where the real work begins.
As a depression therapist in Victoria, BC, Sean uses Acceptance and Commitment Therapy (ACT), a modality with strong evidence for depression that works through values reconnection and behavioural activation rather than waiting for motivation to return. Published research in the Journal of Contextual Behavioral Science supports ACT’s effectiveness for persistent low mood and emotional numbness.
Whether you call it depression, burnout, or just feeling numb, Sean offers counselling for depression in Colwood and across Greater Victoria, with virtual sessions throughout British Columbia. Sessions are covered by most extended health plans through the CCPA. Book a session.